Let's be honest, ulcers aren't exactly the hottest topic at dinner parties. They’re like that unwelcome guest who barges into your digestive system and overstays their welcome. But knowledge is power, and a little humor never hurts anyone—unlike ulcers. So buckle up as we take a deep dive into these troublesome stomach sores.
Ulcer 101
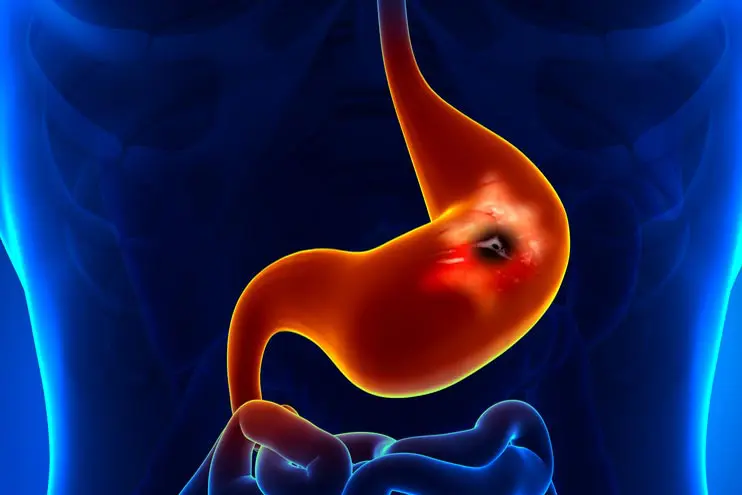
An ulcer is essentially an open sore that develops on the lining of your stomach, small intestine, or esophagus. Think of it as a pothole in your digestive highway—painful, inconvenient, and definitely not part of the original blueprint. The most common types include:
- Gastric ulcers – Located in the stomach
- Duodenal ulcers – Found in the small intestine
- Esophageal ulcers – Affecting the esophagus
It’s Not Just the Spicy Food
Remember when spicy food and stress were blamed for ulcers? Science has since set the record straight. The real culprits include:
- H. pylori bacteria – These microscopic troublemakers are the leading cause of ulcers. Think of them as those noisy neighbors drilling holes in your walls at dawn.
- NSAIDs (Non-Steroidal Anti-Inflammatory Drugs) – Medications like aspirin and ibuprofen can wear down your stomach lining. It’s one of those ironic “the cure is worse than the disease” situations.
- Excessive alcohol consumption – Your wild weekends may be fun, but your stomach lining isn’t celebrating with you.
Do I Have an Ulcer?
Wondering if you've joined the ulcer club? Here are the telltale signs:
- A burning sensation or pain in the abdomen
- Feeling overly full or bloated
- Frequent belching and acid reflux
- Nausea and occasional vomiting
- Unexplained weight loss (not the kind you were hoping for)
Treatment Options
The good news? Ulcers are highly treatable with the right medical interventions and lifestyle changes.
A. Antibiotics
If H. pylori bacteria are to blame, a 10- to 14-day course of antibiotics (often paired with acid-reducing medications) is prescribed. Sticking to the full regimen is crucial to prevent recurrence.
B. Acid-Reducing Medications
- H2 Blockers (e.g., famotidine) – Reduce stomach acid production to aid healing.
- Proton Pump Inhibitors (PPIs) (e.g., omeprazole) – More potent than H2 blockers, they significantly decrease acid production, especially in severe cases.
C. Lifestyle Adjustments
- Avoid irritants like caffeine, alcohol, and smoking, which can delay healing.
- Stick to balanced, non-spicy meals to minimize stomach irritation.
- If possible, avoid NSAIDs and opt for acetaminophen instead (after consulting your doctor).
How to Prevent Ulcers
Prevention is always better than treatment. Here’s how to keep ulcers at bay:
A. Practice Good Hygiene
H. pylori bacteria spread through contaminated food and water. Wash your hands regularly, especially before eating.
B. Use NSAIDs Wisely
Take NSAIDs with food or milk to minimize stomach irritation, or discuss safer alternatives with your doctor.
C. Limit Alcohol & Quit Smoking
Excessive alcohol weakens the stomach lining, and smoking impairs healing. Cutting back significantly lowers your risk.
D. Manage Stress
Chronic stress doesn’t directly cause ulcers, but it can make symptoms worse. Incorporate relaxation techniques like deep breathing, yoga, or regular exercise to support digestive health.
E. Get Regular Check-Ups
If symptoms persist, consult a healthcare provider to prevent complications and receive proper treatment.
Conclusion
Ulcers are a pain—literally—but they don’t have to take over your life. With proper treatment and smart lifestyle choices, you can take back control and show your ulcer who’s boss.
And remember, while this article is informative and maybe even a little entertaining, it’s not a substitute for professional medical advice. So, if your stomach starts staging a rebellion, see a doctor. After all, I might be funny, but I don’t have a medical degree hanging on my wall!